What Causes Diabetes?
What Causes Type 2 Diabetes ?
Type 2 diabetes mellitus is a condition where the body is unable to efficiently convert blood sugar to energy for use and storage. Now, it appears that the brain is the control center for blood glucose management. Before it was believed that the pancreas, the liver and the muscles were the primary decision makers in blood glucose management.
There appears to be a link between obesity and multiple causes of insulin resistance which leads to Type 2 diabetes.
- Dr. Gerard Karsenty of Columbia University found that the bones of the body appear to secrete a hormone calledosteocalcin to signal to fat cells and the pancreas. Osteocalcin has shown the ability to influence how mice secrete and use insulin to move sugar from the blood into the cells and the liver.
- In 2003, researchers noticed large amounts of macrophages in obese lab mice. Macrophages are immune cells that causes inflammation. There may be a link between Type 1 diabetes and macrophages, because it is believed that Type 1 is caused by the immune system (macrophages) destroying all of the beta cells that secrete insulin.
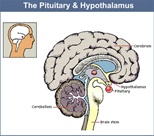
- Around 1850, a French researcher Dr. Claude Bernard damaged the hypothalamus of lab animals in an effort to disrupt their ability to process glucose. More recently, researchers learned that when lab mice lacked insulin receptors in their brains, they also lacked the ability to regulate insulin secretion and efficient use of insulin to convert glucose to energy. Insulin receptors are protein ‘hooks’ found on the outer walls of cells to which insulin attaches to allow glucose and fatty acids to enter.
- Other researchers have shown that free fatty acids communicated directly with the inner part of the brain called the hypothalamus (brain). The hypothalamus controls appetite, thirst, and other drives. Free fatty acids are the simplest form of fat that are taken out of the bloodstream and guided into the cells for processing.
- Leptin, a hormone produced mostly by white fat cells also communicated directly with the hypothalamus. Leptin helps regulate energy intake and energy usage by controlling appetite and metabolism. Leptin numbers increase with the increase in fat cells. Leptin is also secreted by brown fat cells, the placenta, ovaries just to name a few.
- Recently, other researchers have discovered that glucose itself signals directly to the hypothalamus. The hypothalamus signals to the liver to produce and release more glucose into the blood stream if it does not sense the presence of glucose.
- Finally, hormones called incretin secreted by the small intestines signal to the hypothalamus and pancreas to control the amount we eat, our glucose management, and weight loss . Two examples of incretin are Byetta which mimics incretin’s behavior and Januvia which protects incretins like GLP1 from being destroyed.
The hypothalamus area of the brain appears to be the main decision maker as far as glucose management is concerned. As a result many researchers are testing ways to deliver the right signals to the hypothalamus of people with diabetes – a very direct way to control the secretion of insulin and improve blood glucose levels.

The New York Times article dated October 16, 2007



